Plantar fasciitis affects nearly 1 in 10 people but is often used as a catch-all term for pain near the heel. I laid out four key indicators to determine if you have plantar fasciitis or not.
In last week’s blog – part 1 of this three part series on plantar fasciitis – I dove into what plantar fasciitis is, what’s happening at the tissue level, and mentioned that not all pain on the bottom of the foot is actually plantar fasciitis. It’s often used as what I call a “garbage term” where any pain on the bottom of the foot is lumped into a diagnosis of plantar fasciitis. However, accurate diagnosis informs accurate, targeted treatment and therefore quicker recovery.
In an ideal world, if you’re having foot pain, I’d highly recommend getting evaluated by a trusted medical provider but this isn’t an ideal world so I’ve laid out four potential signs of plantar fasciitis. You may or may not have all four but it should give you a better idea of what you’re dealing with.
1 – Location of the pain
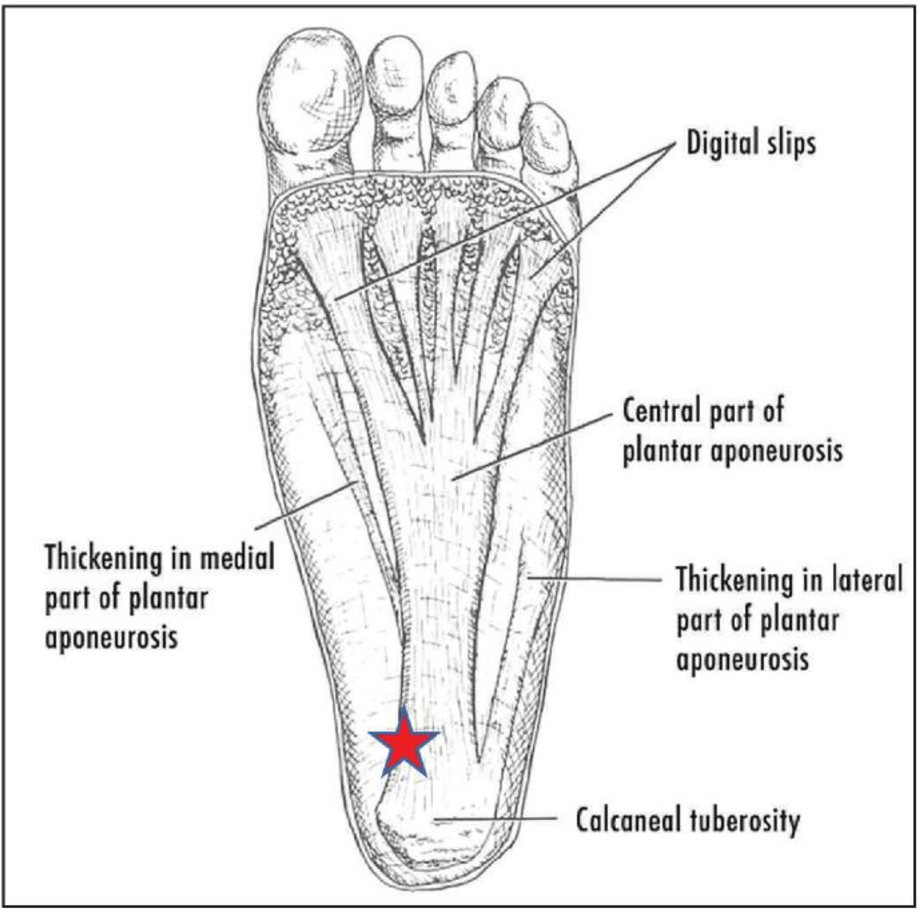
The most common spot – by far – for plantar fasciitis is the medial insertion of the plantar fascia on the heel. A picture is worth a million medical words so here’s two million:
If your pain is on that spot, it’s very likely plantar fasciitis. If it’s more into the heel pad, farther to the outside of the foot, or farther up the foot, it could be a number of other things. That specific location is the highest indicator of plantar fasciitis.
2 – Timing of the pain
With plantar fasciitis, it’s most typically painful for the first steps in the morning, subsides, and then flares up again after some level of activity – being on your feet for x amount of hours – or inactivity – sitting at your desk for x amount of hours – after which, the initial steps are again painful.
It’s typically most painful in the AM because you’ve been in bed without any movement which means the tissue has been static for the same amount of time. When you go to take that first step, the fascia now has to stretch out for the first time in awhile leading to irritation. Same thing when you’ve been sitting or inactive for awhile.
The plantar fascia becomes painful after a certain level of activity because it’s ability to handle stress and load has decreased due to the injury. Therefore, whenever your level of activity is higher than the stress it can handle, the fascia becomes irritated and painful. That’s why one of the best methods to alleviate plantar fasciitis is through targeted strengthening and endurance of the plantar fascia (more on that in part 3 – treatment).
3 – Self tests
At the clinic, there are specific tests that I’ll use to parse out out plantar fasciitis but for at home testing, there are two that I recommend (and only do the second if the first one doesn’t trigger any pain).
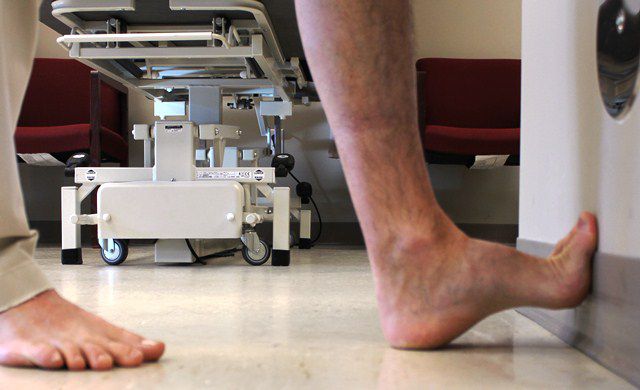
The first test aims to tension the plantar fascia by using a wall to pull back the toes (toe extension).
If you remember from part 1, the plantar fascia attaches to each toe on the bottom of your foot so pulling them back stretches the tissue. If you feel irritation with this test, especially on the inner part of the heel, it’s a good sign you have plantar fasciitis.
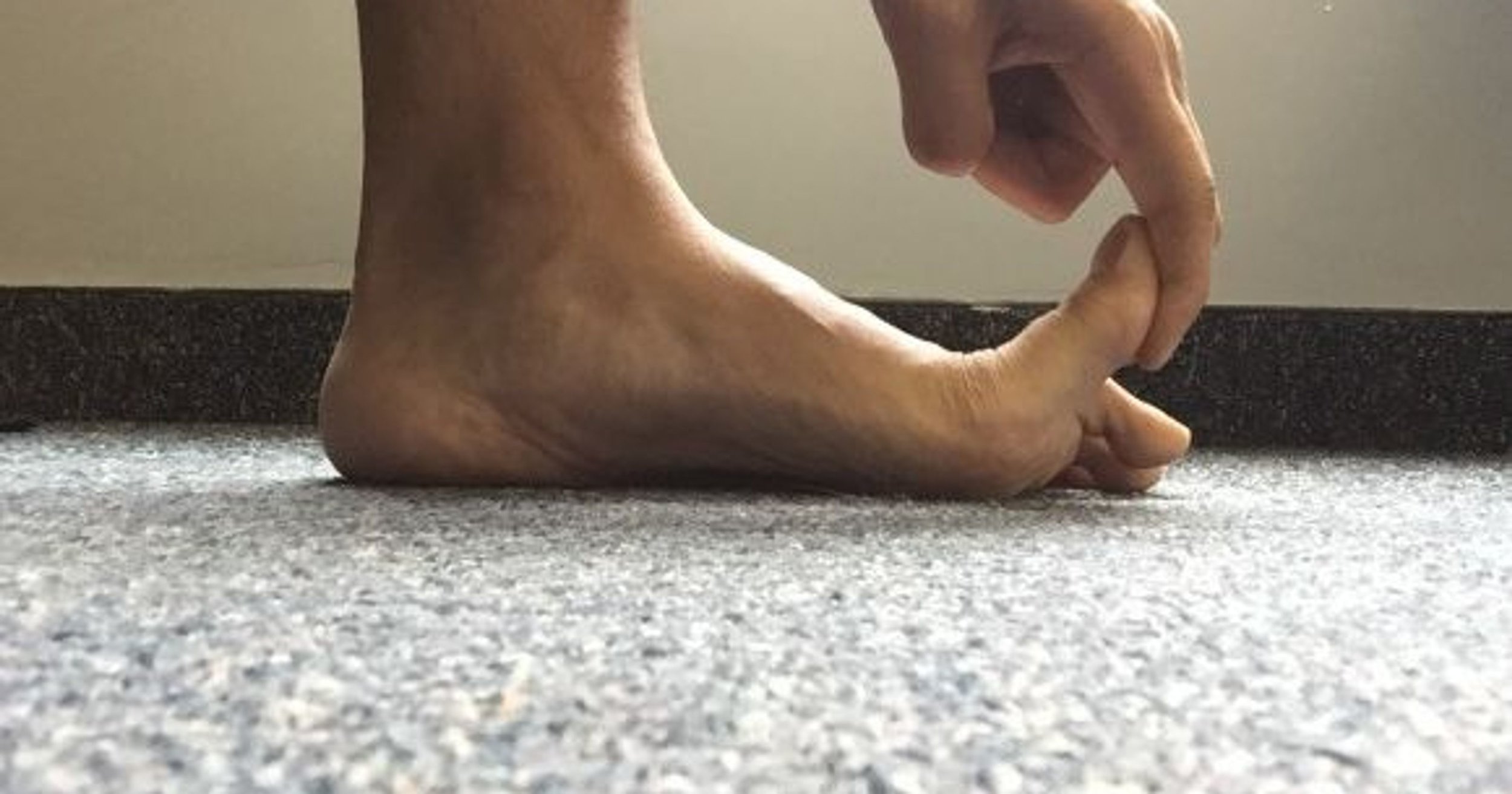
If that test isn’t painful – and it very well may not be unless your plantar fascia is really irritated – then you can do what I call the “crouch test”. Using a wall or counter for balance, put your weight onto the balls of your feet and then slowly crouch down without allowing your heels to drop.
This stresses the plantar fascia with your body weight, it’s far more provoking than the first test. Again, if you feel irritation with this test particular on the medial aspect of the heel, it’s a sign you might have plantar fasciitis.
4 – Limited hallux extension aka a stiff big toe
Something I’ve found with many patients with plantar fasciitis is that if you compare their big toe extension range of motion side to side, the side with plantar fasciitis will be significantly less and feel stiffer.
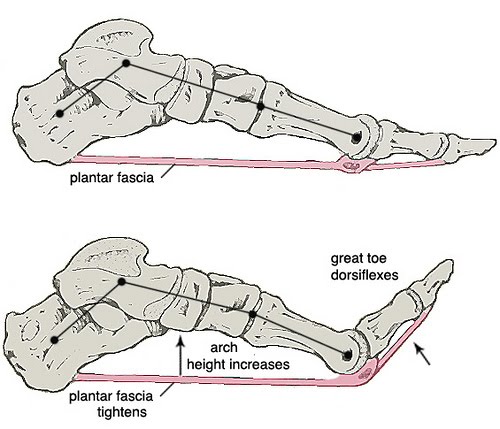
The reason for that is again rooted in the mechanics of the foot and plantar fascia. I spoke about the “Windlass mechanism” in part 1 where coming onto the ball of your foot during walking, running, jumping etc creates big toe extension which passively tightens the plantar fascia and helps stabilize the foot.
If that big toe is lacking extension, that Windlass mechanism isn’t as effective which means increased stress on the plantar fascia to actively stabilize the foot. Over thousands of repetitions (steps, jumps, hops, etc) that can lead to overstressing the tissue and therefore irritation.
These four signs are indicators I very commonly see in patients suffering from plantar fasciitis, particularly #1 and #2. Now that you have a better idea of whether you have plantar fasciitis or not, we can move onto how to actually treat it and get rid of it. That’s for next week.
Thanks for reading and always remember that health and performance are two sides of the same coin.